Child and adolescent mental health services (CAMHS)
for parents and carers
This resource looks at child and adolescent mental health services (CAMHS). It is written for parents and carers whose children might be being treated by these services or moving on from them. It also contains helpful information for children and young people.
About our information
We publish information to help people understand more about mental health and mental illness, and the kind of care they are entitled to.
Our information isn't a substitute for personalised medical advice from a doctor or other qualified healthcare professional. We encourage you to speak to a medical professional if you need more information or support. Please read our disclaimer.
“CAMHS is the first place I really felt I could talk and that I would be listened to.” Jack
Child and adolescent mental health services (CAMHS for short) are mental health services for young people.
These services can help children, young people and their families with a wide range of mental health conditions, neurodevelopmental conditions and behavioural problems.
CAMHS can usually be accessed by young people until they turn 18 years old. Some CAMHS are able to see young people until they are 25 years old.
You might also hear CAMHS being called children and young people’s mental health services (or CYPMHS).
CAMHS is not the only place that children and young people can get support. They can also get support from the following services. If your child is assessed by CAMHS, they might suggest that your child would be better supported by one of these services instead of, or as well as CAMHS.
Their GP
Your child’s GP can help to refer your child for psychological therapy. They can also direct them to other NHS or voluntary services that might be helpful.
Hospital services
Some 16-18-year-olds may be able to access talking therapies through their hospital service.
Their school
Schools can help to support young people with mental health needs, and can refer them on for further support. Some independent schools provide their own therapists who are not connected directly to NHS organisations.
Local charities or support groups
Ask your GP for information about charities and groups local to you and your child.
Local authorities
Some local authorities offer parenting programmes to parents with young people with additional needs like intellectual disabilities or neurodevelopmental conditions. These can help parents to understand more about things like behaviours that challenge and sleep problems. These programmes might be offered by different services in different areas in the UK.
Adoption and looked after children services
These services are for children in care (looked after children) and adopted children. They may be able to direct foster parents, carers and adoptive parents to the help they need. Sometimes adoption services can also offer therapies to parents and young people.
Whether or not your child needs CAMHS instead of another service depends on:
- the challenges they are having
- what kind of support is available where you live
- any other support they have around them
- the referral criteria of your local CAMHS. This is criteria that has been agreed by local services with their Trust and created with reference to national guidance.
In general, young people are referred to CAMHS if they are struggling with their mental health and wellbeing, and:
- other kinds of support haven’t worked
- other kinds of support aren’t available
- they are at risk to themselves or others, and that risk needs specialist support
- they have other factors that might be making it hard for them to cope, or that might mean they need more specialist support. For example, if they also have a neurodevelopmental condition or learning disability.
There are lots of different ‘paths’ that young people can take in interacting with CAMHS. Here are some examples:
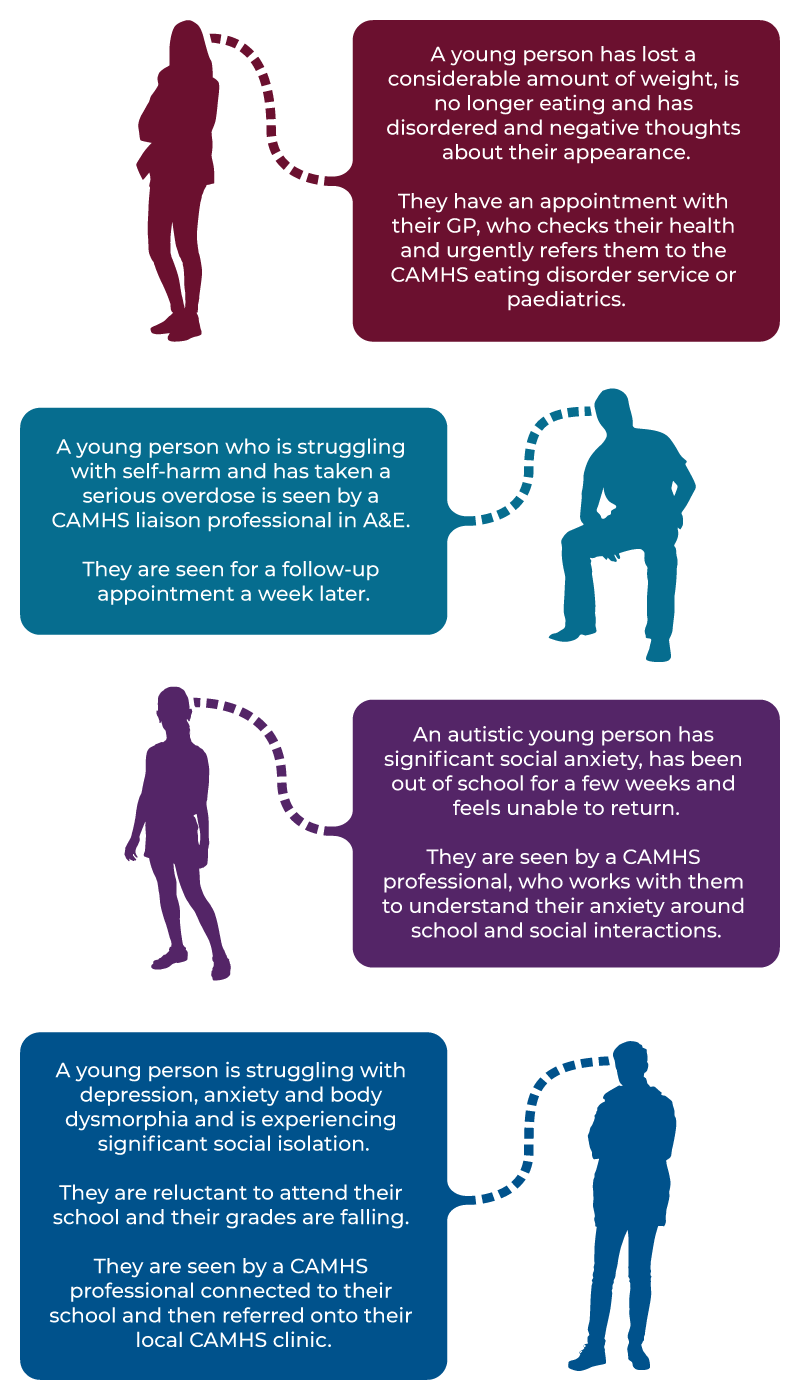
A text alternative to this infographic is also available.
Each CAMHS will have a range of services on offer, and resources available during and outside of their working hours. To understand what is available locally, we recommend that you look at the website of your local CAMHS.
Your child may move between CAMHS services or have several CAMHS services involved at the same time. These services are known by different names in different parts of the country.
Some of the services you might see in CAMHS are listed here. However, these might not all be available where you live:
Triage
The triage or ‘initial treatment’ team helps to signpost young people and their parents to the right services. They may be able to provide you with additional resources.
Mental health support
Some schools have a CAMHS team in them that can provide support directly to young people at that school.
Liaison
You might meet a liaison team if your child goes to A&E or is admitted to a paediatric ward. Some larger hospitals have psychologists attached to their medical teams.
Eating disorder
These are community and inpatient services for children and young people with eating disorders.
Intellectual disability
These are services designed for children and young people who have an intellectual disability (also known as a learning disability).
Neurodevelopmental
These are services for young people who are being referred for an autism or ADHD assessment, or for the treatment of ADHD. Sometimes these services are provided by community paediatrics rather than CAMHS. Paediatricians are medical doctors who specialise in the treatment of children.
In-patient
Some children and young people may need to be admitted to hospital to get the treatment that they need. This is called being an ‘in-patient’.
They might be admitted to a general paediatric ward, a general adolescent unit, or a high dependency unit. These services are specifically for young people who are experiencing mental health difficulties and need a level of care and treatment that cannot be provided to them at home (also known as being ‘in the community’).
You can find out more about inpatient services on the Young Minds website.
Urgent or outreach care
These are intensive services for young people who are in crisis and need more care than can be provided by community CAMHS. Often these services offer out-of-hours or extended-hours care.
Early Intervention in Psychosis
These services are for young people and adults who are experiencing their first episode of psychosis. They often work alongside other CAMHS and adult community services.
Transition
These services help young people to move on, or ‘transition’ from CAMHS to another service.
If your child is struggling with their mental health, they might be referred for a CAMHS assessment. CAMHS assessment referrals can be made by lots of different people, including:
- schools
- GP services
- social services.
In some parts of the UK parents, and young people themselves, can make a referral for a CAMHS assessment. CAMHS assessment referrals can be made until a young person turns 18 years old.
Your local CAMHS will have a referral form or referral portal on their website. This will have specific questions about what help the person filling in the form is looking for, and the challenges the young person and their family are experiencing.
CAMHS will ask for the consent of parents or carers before they accept a referral from a young person to their services. For older children, CAMHS will ask for their consent before they accept a referral made by a parent or carer.
A CAMHS assessment is a meeting, or series of meetings, between a young person and one or more professionals from CAMHS. Sometimes the young person’s parents or carers will attend the assessment as well. This will depend on how old the young person is and what they prefer. These meetings might take place in person, online, or over the phone. This will depend on what you and your child prefer or what is convenient.
“It can be one of the most daunting things to do as you open yourself up to be heard and listened to, to build relationships and talk about the most difficult things and experiences.” Daniel
What happens in a CAMHS assessment?
Preparing for the assessment
Once you get a date for a CAMHS assessment, you might want to prepare by making some notes or thinking about:
- the concerns you have surrounding your child’s mental health
- any changes you have noticed in their behaviour.
It can be useful to bring your child’s 'personal child health record' (their red book) to this appointment. This is because the CAMHS clinician might ask you about your child’s birth and early developmental history. Knowing your family tree can also be helpful.
We understand that you and your child might find it daunting coming to CAMHS for the first time. Your CAMHS team should explain what will happen in the assessment, what to expect and any time frames.
During the assessment
“I was worried about what my initial assessment would be like, but I felt very comfortable as I was offered stuff to support my sensory needs as well as being asked about the lights and chairs in the room. I liked that I was able to sit on a beanbag and use fidget toys. This helped me feel more relaxed so I could think about the questions I was asked”. Lily
A CAMHS assessment typically takes place over several appointments.
Depending on their age and maturity, your child might be offered the choice of being seen on their own. This is because it might be hard for them to discuss their worries honestly in front of their parents or carers. However, if this happens they would still continue to have joint appointments with their parents or carers. Sometimes clinicians will also have appointments with only the child’s parents or carers.
What will be discussed in the assessment?
In the assessment, CAMHS professionals will try to find out more about the concerns you and your child have, and also spend time understanding:
- What your child needs and how they feel. This is called a clinical formulation.
- You and your child’s expectations and needs. They will also try to understand whether you and your child’s expectations and needs are different and, if necessary, if these differences can be resolved.
- The system around your child, such as their school, friends, family and community.
- Your child’s early development, and social and educational history.
- Any other health issues that are affecting your child, you, or any other family members.
You will also discuss how CAMHS might be able to help, or if there are other services your child could benefit from instead of, or as well as, CAMHS.
The main goal of the CAMHS assessment team is to create a safe space for you and your child so that you both feel able to share difficult feelings and experiences. As a parent, it’s important that you try to be as clear and as accurate as possible.
Professionals will be sensitive to cultural and religious differences when working with you. The professionals doing the assessment will also discuss consent with you. This includes explaining who the assessment will be shared with and why.
The assessment can be an important opportunity for you all to ask questions, have time to share some of the worries you have, and feel heard and listened to.
Feeling heard without judgement, sometimes for the first time, can have a powerful effect on the young person and their family.
What questions will my child be asked in the assessment?
The types of questions your child might be asked in an assessment include:
- Who lives in your home?
- Which school or college do you attend?
- What is your education history?
- Who are the important people in your life?
- What are your likes and dislikes?
- What are your strengths?
- What are your worries and concerns?
- What are your eating, sleeping and self-care habits like?
- What has changed to bring you to CAMHS?
- Are there any serious events in your life that have happened recently?
- Are you hurting yourself or are you feeling suicidal?
You or your child might be concerned that an ‘assessment’ means that coming to CAMHS is like taking a school test or having an interview that you need to do well in. Don’t worry, an assessment in CAMHS means that the people you are speaking to are gathering information about your child. There are no right or wrong answers, and there are no ‘stupid’ questions.
“As a parent it’s easy to worry that you haven't done enough, or think ‘did I bring them in in time?’” Abiola
“We had a long wait to get into the service but once we did it was a big relief to finally get some help. I was glad that I was asked if I wanted my mum in the assessment with me or not. This made me feel like I was part of the process and not just looking on.” Aisha
The CAMHS team will work with you and your child to develop a care plan. This plan will include:
- The outcome of your initial assessment.
- Your shared understanding of the next steps.
- Goals that you and your child want to work towards.
- A risk plan or safety escalation plan, if this is necessary.
- Which clinicians will be your child’s key worker, or the main people you can contact about your child’s care.
- Out-of-hours emergency contact information.
Each service is different, but you will usually be given a physical copy of this information.
If your child’s treatment plan includes psychological therapy, your child may have to wait to receive this. You might be told that they are on a ‘waiting list’. How long they have to wait will depend on where you live and your child’s symptoms. It is important that you let the CAMHS team know if there are any changes while you are waiting. They might be able to direct you to other support services while you are waiting.
What if the referral is declined by CAMHS or we are signposted to a different service?
You and your child might feel disappointed if this happens. It is important to remember that this does not mean that your child is ‘not unwell’, that they are ‘not at risk enough’, or that they will receive a lower standard of care.
Your CAMHS assessment team should explain why your child has not reached the referral criteria for their service, and what other service they feel could help to support your child better.
If your referral is accepted, the CAMHS team will offer your child different kinds of treatment and support. What these are will depend on your child’s needs, what is available at the CAMHS you have been referred to, and the feelings you and your child have about different treatments.
Psychological therapies
This is the main treatment for young people referred to CAMHS services. There are lots of different kinds of psychological therapies, and the kind your child is offered will depend on the challenges they are experiencing.
Some examples of psychological therapies are:
- cognitive behavioural therapy (CBT)
- dialectical behavioural therapy (DBT)
- family therapy
- art therapy.
Medication
There are lots of different medications that can be used to treat mental health conditions. The CAMHS team will tell you if they think that your child might benefit from taking medication.
You and your child will have the opportunity to discuss how these medications work, any side-effects to expect, and what to do if your child experiences these.
The professional that prescribes the medication to your child should give you a leaflet that contains information about the specific medication. There are usually different formats including easy read versions, and many have been translated into different languages. Read this information and ask your prescriber if you have any questions.
Occupational therapy
Occupational therapists can support young people with practical things, like their daily routines. They can also assess how a young person manages different tasks. For example, handling money, using public transport, or going into shops. They can be particularly helpful for young people with learning disabilities or neurodevelopmental conditions.
Peer support
Peer support is where someone gets support from another person with similar experiences to them. In CAMHS, there might be peer support groups where young people can talk about their feelings and learn from other people who are further along in their recovery.
Other support
Other kinds of support include:
- dietary support
- speech and language therapy
- family therapy
- physical and mental health monitoring
- general support from support workers.
“I got support for myself and later also for my family. I think it is important to remember the impact this can have on siblings and was glad that I was offered family therapy. It really helped me to engage with my treatment and stay connected to my sister at a difficult time.” Lily
Every CAMHS is different, and team sizes can vary. Some clinicians will have multiple roles, and your child might be seen by a number of different CAMHS professionals. These professionals have a range of psychological skills to support your child. They will consider the systems around your child and family when they develop their care plan with you.
“I had support from lots of different CAMHS teams. This started when I was admitted to hospital. Some came to my home, some I saw for appointments at clinics. At the time I never really thought about it but having all that different support, depending on how unwell I was, helped me a lot”. Jack
Key worker
Every child or young person in CAMHS has a key worker. This is also sometimes called a care coordinator, case manager or core worker. This person will take the lead role in organising your child’s care, sometimes with the help of other roles in CAMHS. They will also act as the main point of contact for your child and your family.
A key worker can be one of a number of different roles within the CAMHS team. Who your child’s key worker is will depend on lots of things, including:
- the kinds of challenges your child is experiencing
- the skills and training that key worker has, and how these relate to your child’s needs
- what roles are available at the specific CAMHS
- the availability of different staff when your child is referred to the CAMHS team.
You and your child have the right to request a change in their key worker if you feel that they are not building a positive relationship with that person. While this request cannot always be fulfilled, it will always be considered.
Other roles
- Clinical psychologists – They can assess young people and provide them with different kinds of support for their mental health problems.
- Psychotherapists – They provide different kinds of psychological therapies, such as art therapies and family therapies.
- Child and adolescent psychiatrists – These are medically qualified doctors that specialise in working with young people with mental health problems and their families. They can also prescribe medication.
- Specialist mental health nurses – These are nurses who work in hospitals and the community, to support people with mental health conditions. Some nurses called ‘non-medical prescribers’ can also prescribe medication.
- Social workers – Some CAMHS professionals have a background in social care. They will be experienced in considering the psychological, social and systemic issues that could be contributing to your child’s mental health problems.
- Allied health professionals – These are healthcare professionals who specialise in particular treatments and practices. They include roles like dieticians, physiotherapists and occupational therapists.
- Paediatricians – These are doctors that specialise in diagnosing and treating babies, children and young people with physical health conditions and some neurodevelopmental disorders. They work closely with some CAMHS teams.
- Support workers – They work with other healthcare professionals and support them to treat their patients.
Remember, these roles might have slightly different names in your service. Usually, your CAMHS will have a list of who is in their team on their website. If you or your child have access needs, you can also ask for photographs and printed information about the professionals you are seeing.
Any people you meet in CAMHS should explain who they are, and what role they are taking in your child’s care.
All of the people that your child sees will have a variety of skills in assessing and treating mental health problems in young people. For example, your child might see an occupational therapist who might also have training in giving psychological therapies.
“From my experience, there can be a lot of anxiety around CAMHS, from other parents sharing things. One person might say ‘my child is seeing a practitioner in this role’. And you might think, ‘oh, my child isn’t seeing a practitioner in that role’. It’s important to remember that it might be called something different in your CAMHS, but be the same role.” Abiola
Why is my child seeing a psychiatrist?
There are some misunderstandings about the role that psychiatrists have in CAMHS. These include:
- that your child’s mental health will only be taken seriously if they see a psychiatrist
- that if they are seeing a psychiatrist this means that their mental health problems are severe
- that if they are seeing a psychiatrist they will be prescribed medication.
There are lots of different reasons that psychiatrists work with children in CAMHS. The main reason your child might see a psychiatrist is that they are able to provide a different perspective on their mental health, and the treatments and support that might be helpful to them.
Your child’s psychiatrist should consider any biological, psychological and social factors that could be contributing to your child’s mental health challenges.
CAMHS services will always share your information with your GP. This is because your GP is the central point for your clinical records.
With you and your child’s consent, CAMHS might also meet with other services. This is called ‘multiagency working’. Which services CAMHS meets with will depend on the help your child is receiving and the challenges they are having, but could include:
- education providers such as your child’s school
- voluntary sector organisations and charities
- social care services.
Occasionally, if there are significant concerns about your child’s wellbeing or the wellbeing of others, CAMHS may need to share information without you or your child’s consent. The CAMHS team will talk to you and your child in detail about this if it happens.
How much you will be involved in your child’s care, and how much your child is involved in making decisions, will depend on lots of different things. These include:
Whether they are able to give informed consent
Informed consent is when a young person:
- is given clear, accessible information about their possible treatment and care plan
- has the capacity to understand, retain and make decisions based on that information
- and can communicate their decision to a CAMHS professional.
Some young people are unable to consent to their suggested treatment plan. If this is the case it might be more appropriate for their parents or carers to make these decisions for them. Ideally you and your child will make these decisions together.
Whether or not a young person is able to give consent to a treatment can change over time. It will depend on a number of factors such as their age, development, and whether they have a mental illness.
Consent has to be constantly assessed. This means that even if a child cannot give consent for one thing, they may still be able to give consent for other things.
How much they want you to be involved in their care
The Mental Capacity Act 2005 says that young people aged 16-18 should be presumed to have the ability to make their own decisions, including consenting to medical treatment, unless they lack the capacity to do so.
While parents continue to hold parental responsibility for children under 18, their decisions cannot override the decisions of a ‘competent’ 16 or 17‑year‑old.
As your child gets old enough to start making their own decisions, healthcare professionals will start to seek your child’s consent before they share their personal information.
Some young people will request that their information is not shared with their parents. If this happens, and they have been assessed as able to make that decision, their confidentiality will be respected and upheld by the CAMHS professionals.
CAMHS professionals will be clear with the young person if there are times when this confidentiality needs to be broken and their information needs to be shared with others, such as their parents. This might be necessary if there is a real and serious risk to the health, safety or welfare of your child, or another person.
It is important to know that, as a parent or carer, you will always be able to share your thoughts and concerns with the professionals working with your child. Confidentiality should not prevent contact between professionals and carers, or prevent professionals from listening or receiving information.
“As a parent, I can’t overstate how important it is for professionals to work closely with families. Especially when treatments or medications are changing. We know our young person better than anyone, and when clinicians truly listen and involve us, it makes the whole process safer, calmer, and far more effective. It feels like we’re navigating things together rather than alone.” Toni
“I felt very nervous about leaving and that it was going to come sooner than I was ready. However with a lot of reassurance and a few extra sessions I felt ready.” Lily
Leaving CAMHS (also known as ‘discharge’) will be a decision that is made between you, your child and the CAMHS team. It will happen after your child has received the care in their care plan or has recovered sufficiently.
Your child might transition into another service when they are discharged. For example, they might reach the age of being ready to leave CAMHS (16-18 years old) but need further treatment from the adult mental health team.
In preparing for leaving CAMHS, the following things might be discussed with you and your child:
- Your child’s mental health needs.
- Your child’s treatment plan and how to continue with the skills that they have learnt in CAMHS.
- Early warning signs which might indicate that it is time to request a re-referral to mental health services.
- Whether your child needs to be referred to adult mental health services, or another service.
What is it like leaving CAMHS?
How you and your child feel about leaving CAMHS will depend hugely on you as individuals, and the circumstances for why your child is leaving CAMHS.
You and your child should be given a lot of time to adjust before it is time for your child to leave CAMHS or move onto another service. You should be informed about what other kinds of support will be available to you and your child when they leave CAMHS.
If you have any concerns about your child leaving CAMHS, or being discharged from mental health services, speak to your key worker.
“I think it’s helpful to plan in advance for what it will look like, so it’s not too sudden.” Abiola
“Watching my child move from CAMHS to adult services felt like standing at the edge of a cliff. For years we had support, structure, and people who knew our young person. Then suddenly, at 18, everything changed. Families need professionals who don’t let our children fall between the gaps, and who make the transition feel like a handover.” Toni
How quickly will this happen?
Leaving CAMHS is usually planned over a few sessions. Being discharged from CAMHS can take longer if your child needs to transition to a different service, and has to wait to be accepted into that service. Sometimes, your child’s care and treatment might need to be managed by your GP or another service in the meantime.
It is important for healthcare professionals to take into account if your child has any other factors that might make moving on from CAMHS more challenging. For example, if they struggle with change due to neurodiversity. If this is the case, they will support you and your child to make this transition as smooth as possible.
“My key worker spoke to me about being referred on to adult services, but I decided I didn’t want to do this. I felt ready to step away from support and look after myself. We spoke about this several times, which helped me make this decision, and I was given the information on how to make contact later, if I changed my mind”. Aisha
Some young people in CAMHS will be referred to adult mental health services when they turn 18 years old. Unfortunately, there can be delays to your child transitioning to adult services if there are waiting lists.
In adult services, your child will interact directly with their mental health team, and will be sent letters and information about appointments directly. Adult mental health services will still try to work collaboratively with families and carers as they understand that this can improve the care your child receives. However, your child will need to give their explicit consent for this to happen.
As a parent, you might find the move from child to adult mental health services challenging, especially if you are used to being very involved in your child’s care.
“Often when you're a carer, it's been your identity and your experience for such a long time, and then suddenly the staff are liaising directly with your child. So, it is a shift for the parent as well, to have to step back a bit.” Abiola
Some parents and carers may need to be more involved in decision making and information sharing. For example, if a child has additional learning needs, such as an intellectual disability, and lacks the capacity to make certain decisions about their care. If you remain responsible for your child’s care, the adult mental health service will liaise directly with you.
You can find out more about the role of carers in our resource on caring for someone with a mental illness.
“It took a while for me to actually be accepted to an adult mental health service. It’s important to remember it's not because you're not unwell enough or anything, it's just they're trying to find the right place for you.” Emma
Young people and their parents often want to know what happens with the information that they share with mental health services, while they are being cared for by a service and afterwards.
The majority of records are stored electronically. Young people and their carers can speak to their key worker to clarify who has access to their clinical information and how their data is being stored and used.
Data should only ever be shared for a clear purpose. If your child’s data is being shared with other professionals they should usually be informed about this. Very rarely data is shared with professionals without consent. This is usually in the context of safeguarding, and because there is a risk to your child or to others. Even in this case, CAMHS professionals will make every attempt to let you and your child know that this information needs to be shared.
Healthcare professionals have a duty to carefully consider when it is necessary to share information and when it is not.
Making a subject access request
A subject access request is when you or your child make a request to access their clinical records. When children are over the age of 12 or 13, they must give their permission if their parents want to access their clinical records.
Usually, you or your child would make a request to your CAMHS team, who would then signpost you to their Subject Access Request Team or send you a form to complete. The mental health charity Mind have a page on their website that explains how to do this.
Bear in mind that your child’s clinical records will not include any ‘third party information’. This means information that relates to anyone who is not the clinician, patient or carer would be removed from the clinical record.
CAMHS information for 11-18 year olds, Mind – The charity Mind have a CAMHS 'hub' that looks at what CAMHS is and how it works.
Support for parents, Young Minds – The charity Young Minds have a section of their website for parents who are supporting their children with their mental health.
This information was produced by the Royal College of Psychiatrists’ Child and Family Public Engagement Editorial Board (CAFPEB). It reflects the best available evidence at the time of writing.
Clinical experts: Dr Reenee Barton, Emma Lawton and Constance Bowler
Experts by experience: Abiola Johnson and Emma Wakefield
Thank you to the young people from the Somerset CAMHS Participation Groups for sharing their experiences as quotes in this resource. Their names have been changed throughout.
Full references available on request.
Published: April 2026
Review due: April 2029
© Royal College of Psychiatrists











