Post-traumatic stress disorder (PTSD)
This information is for anyone who has or thinks they might have post-traumatic stress disorder (PTSD), and their friends, family and carers.
About our information
We publish information to help people understand more about mental health and mental illness, and the kind of care they are entitled to.
Our information isn't a substitute for personalised medical advice from a doctor or other qualified healthcare professional. We encourage you to speak to a medical professional if you need more information or support. Please read our disclaimer.
Post-traumatic stress disorder (PTSD) is a mental illness that can develop when someone experiences or witnesses a traumatic event.
Many people who go through a traumatic event will experience a range of negative emotions, thoughts and memories afterwards. For many people, these symptoms will improve with time and support. When these negative feelings don’t go away, and interfere with someone’s daily life, they might be experiencing PTSD.
How common is PTSD?
A national survey found that around one in 20 adults in England screened positive for PTSD. ‘Screened positive’ means that a person completed a mental health symptoms questionnaire to check for the symptoms of PTSD. Their answers to this questionnaire suggested that it is likely they had PTSD.
PTSD can affect anyone who experiences a single traumatic event, or multiple traumatic events. We have given some examples of these events below.
It is important to remember that the events listed below are just examples. There are a huge number of events not covered here that can lead to someone developing PTSD. If your experience is not covered here, it is still valid and you should seek help and support if you are suffering.
Events that can lead to PTSD include, but are not limited to:
- seeing someone die or thinking you were going to die yourself
- being seriously injured, or believing you were going to be
- experiencing sexual violence, or believing that you were going to experience it.
You might be exposed to a traumatic event in one of the following ways:
- Directly – It happened to you.
- Witnessing – You saw it happen to someone else.
- Learning – You found out that the event had happened to someone very close to you.
- Threatened – You experienced a ‘near miss’ event that you thought was going to lead to a serious, terrifying or horrific outcome, but did not. For example, a severe malfunction or incident on a plane that led you and other passengers to believe the plane was going to crash.
We also know that some people who are exposed to traumatic events through social media, television, films or pictures can experience mental health difficulties. This is particularly the case if the exposure occurs as a result of their work.
Some people experience just one traumatic event, but unfortunately many people experience multiple traumatic events. When traumatic events occur repeatedly, in a way that causes someone to feel that they cannot escape future traumas, they might develop a condition called complex PTSD.
There are a huge number of traumatic events, but here are some examples:
- witnessing a violent death
- serious accidents, e.g. a car crash
- physical or sexual assault or abuse
- serious health problems, being in intensive care and other traumatic healthcare experiences
- complicated or life-threatening childbirth experiences
- being diagnosed with a life-threatening or life-changing illness
- war and conflict
- terrorist attacks
- natural or man-made disasters, e.g. tsunamis or fires. Man-made means that something is caused by a person or group of people and doesn’t occur naturally.
If your experience is not covered here, it is still valid and you deserve help and support.
Some events feel traumatic not only because something awful happened, but because we find it hard to make sense of why it happened. Traumatic events often do not fit with our sense of what the world should be like. This makes it difficult for us to understand the meaning behind them and this confusion can affect our mental health.
Traumatic experiences can also show us that bad things can happen to us and the people we care about at any time. This can lead to us feeling unsafe, disconnected and constantly under threat. This is understandably frightening. Sometimes traumatic events can make us question who we are, which can be distressing too.
Many people will experience traumatic events throughout their lives. Around 1 in 3 adults in England report having experienced at least one major traumatic event in their lifetime. However, not everyone who experiences something traumatic will go on to develop PTSD.
Many people experience grief, sadness, anxiety, guilt and anger after a traumatic experience. This does not necessarily mean that they have PTSD. People who have PTSD often exhibit several of the symptoms listed below. These can start immediately, or they might take some weeks or even months to begin.
Everyone’s experiences of PTSD are different. You might have all, some or just a few of these symptoms, and your symptoms might change over time.
With PTSD, these symptoms will interfere with your day-to-day activities and cause you to feel very distressed. If you have any of these symptoms immediately after a traumatic event, this does not necessarily mean you will develop PTSD.
Re-experiencing, or intrusion symptoms
- Memories – Having unwanted memories of the event that are very overwhelming and distressing. These are known as intrusive thoughts. These can sometimes feel like your mind is playing a video of what happened on repeat.
- Nightmares – These are unpleasant dreams, related to the trauma, that wake you up.
- Dissociative reactions – Feeling or acting as if the traumatic event is happening again in real time. This is known as a flashback. You might stop being aware of what is happening around you or feel that the world is no longer real.
- Physical and psychological distress – Feeling very distressed, agitated or overstimulated when reminded of the event in some way. You might breathe quickly, or have a fast pulse. You might not always realise when these emotions have been triggered in you, or what has triggered them.
Avoidance symptoms
- Dissociative amnesia – Being unable to remember parts of the traumatic event. This is a common way that your brain tries to protect you from traumatic experiences. However this can end up making things harder in the long-term. Sometimes as you try to recall parts of the event, you might start to feel disconnected from yourself and the world around you. This is known as dissociation.
- Detachment – Feeling detached from or no longer close to people you previously felt close to.
- Avoiding talking and thinking – Not wanting to speak about, or think about, the traumatic event or events.
- Avoiding associations – Avoiding memories, thoughts, feelings, things, people and places associated with the traumatic event. This might include avoiding TV or other media about the event, especially if it causes you distress.
Changes in your mood and thoughts
- Negative beliefs and expectations – Thinking negatively about yourself, others or the world.
- Blame – Blaming yourself or other people for the traumatic event happening or its consequences, even if you or they were not responsible.
- Negative trauma-related emotions – Persistently experiencing fear, horror, anger, guilt or shame. You might feel angry with other people or yourself, even if neither of you have done anything wrong.
- Loss of interest in activities – Struggling to take pleasure from or be interested in activities that you used to enjoy or do regularly.
- Unable to feel positive emotions – Struggling to experience happiness, satisfaction or feelings of love.
Alertness and reactivity symptoms
- Hypervigilance – Being overly aware of what’s going on around you and being unable to relax because you’re looking for threats.
- Being startled easily – Overreacting to noises or movements.
- Difficulty concentrating – Finding it hard to focus on tasks that you were able to focus on before.
- Difficulty sleeping – Finding it difficult to fall asleep and stay asleep. When you do fall asleep your sleep might be poor or broken, and you might have nightmares.
- Irritability – Having outbursts where you are verbally or physically aggressive towards people or things. These outbursts might happen when you experience something that reminds you of the traumatic event.
- Recklessness – Acting impulsively or in ways that are risky or self-destructive. For example, going into potentially dangerous or violent environments.
There are several possible explanations for what causes PTSD.
Psychological
The psychological symptoms of PTSD are deeply unpleasant and distressing. However, these symptoms can make sense when we think about how our minds might work to protect us after a traumatic event.
Intrusive thoughts or flashbacks
It is completely normal for us to ‘replay’ a difficult or traumatic experience in our heads. This is a natural response that our brain does to help us to understand what happened. It can help us to be more prepared if the situation was to happen again.
However, in PTSD this response becomes too extreme. People with PTSD will re-experience the event again and again through intrusive thoughts or flashbacks. This will cause them to feel extremely distressed, rather than helping them to make sense of what happened.
Avoidance and numbing
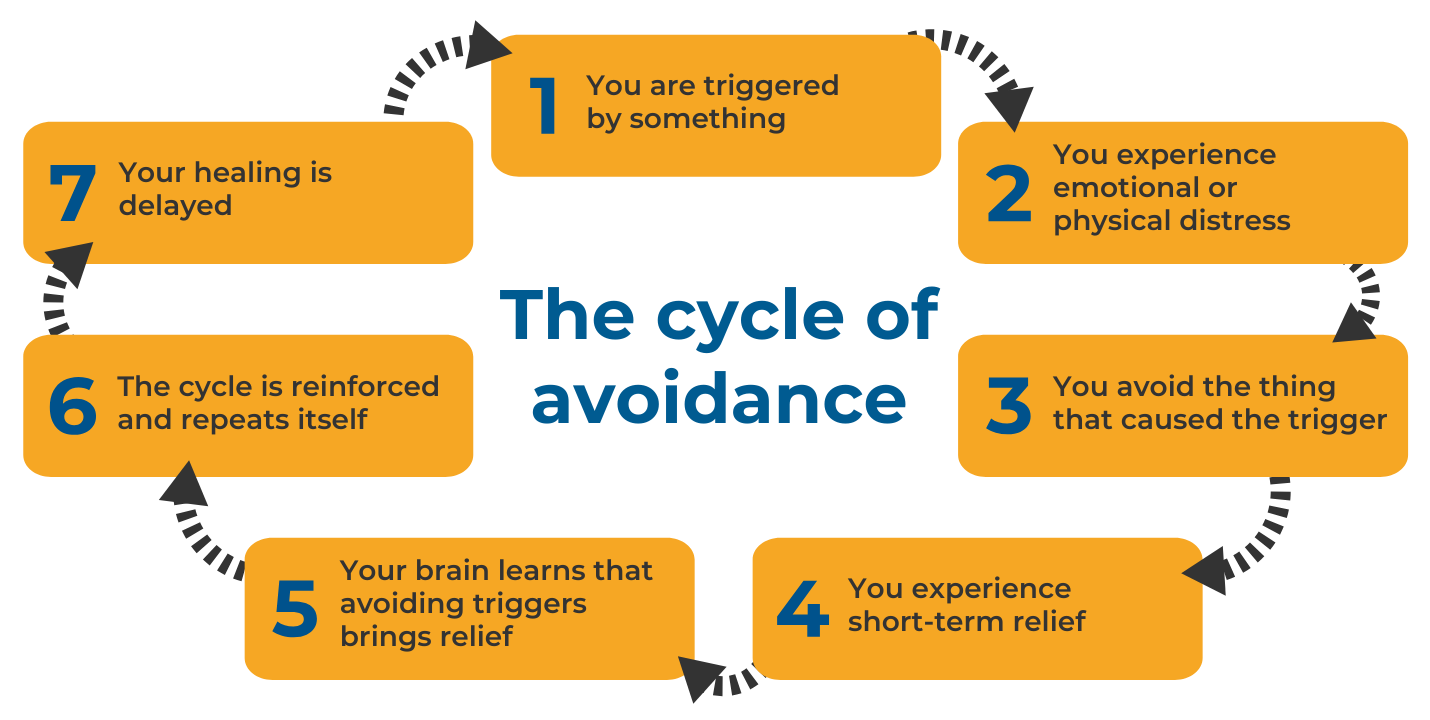
After experiencing a traumatic event we might be unable or unwilling to remember it. While it can be distressing to remember what has happened, reflecting on the event can help us to make sense of and recover from it. If we avoid thinking about the event, the memories can become stronger and more distressing when we do think of them. Below is a diagram showing the cycle of avoidance in PTSD:
Hypervigilance
If we are ‘on guard’ or overly sensitive to what is going on around us, we might feel prepared to react quickly if another crisis happens. This response can also give us the energy to do what is needed after an accident or crisis.
However, in people who have PTSD these feelings happen all the time, long after the threat has passed. The feelings will also happen in situations where the threat could not possibly happen again. This can be exhausting and prevent people with PTSD from doing the things they used to enjoy.
Physical
Some of the physical symptoms of PTSD happen because our bodies are struggling to process trauma. We can become stuck in ‘survival mode’ even after the real danger has passed.
Adrenaline
This is a hormone our bodies produce when we are under stress. It helps to prepare our bodies for activities that need a lot of energy. For example, running or fighting someone off. When the stressful event ends, the level of adrenaline should go back to normal.
For people with PTSD, vivid memories of the stressful event can keep their levels of adrenaline high. High levels of adrenaline can make us tense, irritable, and unable to relax or sleep well.
The hippocampus
This is a part of the brain that processes memories. High levels of stress hormones, like adrenaline, can stop the hippocampus from working properly. This means that memories of the traumatic event aren’t processed correctly. This can cause us to remember the event as though the risk is still present now, rather than something that happened in the past.
People with PTSD often don’t have any of these psychological or physical responses consciously or intentionally. These are automatic responses caused by trauma.
Anyone can get PTSD if they have experienced a traumatic event. However, some people have jobs that mean they are more likely to experience traumatic events. This means the risk of them developing PTSD is more likely than in other careers. These jobs can include:
- emergency service workers (e.g. police officers, firefighters or paramedics)
- social workers
- healthcare professionals (e.g. intensive care staff or midwives)
- military personnel and other professionals and volunteers working in war zones
- train drivers who experience a death on the track
- professional online content moderators who have to view distressing material as part of their job.
The symptoms of PTSD often start immediately, or soon after a traumatic event. Sometimes PTSD symptoms do not start for weeks or even months after the traumatic event. In most cases they start within six months of the event. A delay of six months or more is not impossible, but is much less common.
What is unfortunately more common is that many people will not ask for help when their symptoms first start. This is because it can be hard to recognise what’s happening, or to know when to reach out. People can also fear being judged negatively by others, including their employers.
PTSD should not be diagnosed in the first month after a traumatic event. If you experience trauma symptoms straight away, and these are severe and prevent you from functioning, you might be experiencing an acute stress reaction (also known as acute stress disorder). These symptoms will normally improve or go away within a few days to a few weeks. In some cases you might find it helpful to seek help from a professional.
After a traumatic experience, many people will experience or display some trauma symptoms for the first month or so. These are often normal reactions to experiencing real or perceived danger. You can think about them as your brain’s way of protecting you from harm or part of the process of making sense of what has happened.
However, most people will process what has happened over a few weeks, or sometimes a little longer. As they do so, their distress symptoms will start to decrease in frequency and intensity.
Research shows that certain groups of people are at increased risk of experiencing PTSD. These include:
- People who experience repeated trauma. For example, people who are living in conflict zones.
- People who are already vulnerable because of their past experiences. For example, people who have a history of trauma, such as experiencing abuse during childhood.
However, the risk of developing PTSD is decreased if someone can:
- access good social support and
- recover from the traumatic event in a ‘lower stress environment’.
Workplaces, family and friends can help people exposed to trauma by providing extra support. They can also help by protecting them from experiencing further stress for a little while.
What events are more likely to cause PTSD?
Any traumatic event can cause PTSD. However, you are more likely to develop PTSD if the event:
- is sudden and unexpected
- goes on for a long time
- happens when you are trapped and cannot get away
- is ‘man-made’
- causes many deaths
- causes severe injury or disfigurement (mutilation)
- involves children.
This does not mean that other experiences cannot lead to someone developing PTSD. What feels traumatic can vary greatly from person to person. If you continue to be exposed to stress and uncertainty as you are trying to recover, this can make it more difficult for your PTSD symptoms to improve.
You may have recovered from a traumatic experience if you:
- can think about it without becoming overly distressed
- don’t feel constantly under threat or on edge
- don’t think about it when you don’t intend to
- don’t avoid reminders of the event.
There are several reasons someone with PTSD might not be diagnosed.
Avoidance
People with PTSD will often avoid talking about how they are feeling so they do not have to think about the traumatic event.
Some people feel that the symptoms they are experiencing (for example, avoidance and numbing) are helping them to cope. They might not realise that these are symptoms of PTSD.
Stigma and misunderstanding
When someone is very unwell, they can find it hard to believe that they will ever return to how they felt before the traumatic event.
Some people can minimise their experiences because they believe that others ‘had it worse’. Others might not ask for help because they are ashamed of being unwell, or concerned that others will judge them.
There is a common misunderstanding that only people in the military or emergency services get PTSD. This can mean that people are not believed by others when they share that they think they might have PTSD. In fact, PTSD can happen to anyone, and every experience of PTSD is valid.
Incorrect diagnosis
Some people who have PTSD are incorrectly diagnosed with other conditions. For example, anxiety disorders, depression or personality disorder.
Some people have other psychological or physical health problems that cause their PTSD symptoms to go unnoticed or lead to misdiagnosis.
People who have PTSD might also have ‘medically unexplained physical symptoms’ such as:
- gastrointestinal difficulties
- pain syndromes
- headaches.
These symptoms can mean that their PTSD is identified as a physical symptom or illness. This is why it is important for healthcare professionals to ask about experiences of trauma when they are assessing someone.
Other challenges
Some people with PTSD might also develop other challenges because of their symptoms. For example, relationship difficulties or dependence on alcohol or drugs.
These difficulties might be linked to their PTSD, but they can be more obvious than the PTSD itself. The person with PTSD and those around them might not realise that these problems are a consequence of the trauma they experienced.
PTSD can develop at any age. However, most children who experience traumatic events will not go on to develop PTSD, or any other mental illness.
The symptoms of PTSD in children are similar to the symptoms in adults. Children can also experience:
- Frightening dreams – In children, these dreams may or may not seem directly related to the actual traumatic event.
- Repetitive play – Some children will act out the traumatic event when they are playing. For example, a child involved in a serious road traffic accident might re-enact the crash with toy cars.
- Physical symptoms – They might complain of stomach aches or headaches.
- Fear that their life will end soon – They may find it hard to believe that they will live long enough to grow up, or find it difficult to imagine a future.
Read our trauma and distress resource for parents and carers to find out more.
There are many different and effective treatments for PTSD. The most effective treatments are psychological therapies (also known as talking therapies). Your GP or other healthcare professional might also suggest medication, such as antidepressants.
Psychological therapy
Most, but not all, psychological therapies for PTSD focus on the traumatic experience itself. They will focus less on other events that are happening in your life now or that happened in the past. Psychological therapy will help you with the following things:
- Acceptance – Learning to accept that although you cannot change what has happened, you can think differently about the event, the world and your life.
- Remembering the event – Remembering what happened without being overwhelmed by fear and distress. You will be able to think about what happened when you choose to, rather than through intrusive thoughts or flashbacks.
- Putting your experiences into words – Talking about what happened in a way that helps you to make sense of it, so the memories feel less overwhelming.
- Feeling safer – Helping you to feel more in control of your feelings. This can help you to feel safer, so you will not need to avoid the memories as much.
Any talking therapy for PTSD should be provided by someone who is trained and accredited in trauma-focused therapy. Therapy sessions are usually at least weekly, with the same therapist. You will usually have 8-12 sessions, but you might need more if your PTSD is particularly complex. Sessions will usually last between one hour and 90 minutes.
The most effective psychological therapies for PTSD are:
Trauma-focused cognitive behavioural therapy (TF-CBT)
This is a talking therapy that can help you to change your ways of thinking. In time this can help you to feel better and to behave differently. This is usually delivered one on one between you and a therapist. There is some evidence that TF-CBT can also be delivered in groups.
Eye movement desensitisation and reprocessing (EMDR)
This is a technique that involves moving your focus between the left and right side of your body. This is called ‘bilateral stimulation’. It is usually done with eye movements but there are other ways, such as hand tapping, or alternating sounds. EMDR helps the brain to process traumatic memories to make them less distressing.
You will be asked to recall the traumatic event and how it makes you think and feel. While you do this, you will be asked to perform the ‘bilateral stimulation’. This has been shown to lower the intensity of the emotions you experience around a traumatic memory. This can help to resolve the trauma.
EMDR should be delivered by a qualified and accredited practitioner. EMDR is usually given over 8-12 sessions. Each session lasts between one hour and 90 minutes.
Other treatments
Some other forms of talking therapy may help to target specific symptoms (e.g. poor sleep). These can be helpful for people who do not respond well to TF-CBT or EMDR.
Whilst there are many therapies that claim to treat PTSD, you should be cautious about using them unless the risks and benefits have been properly explained to you.
There is some evidence to suggest that briefer, non-trauma-focused therapies might be helpful for some people. However, currently the best evidence of effectiveness for treating PTSD is for TF-CBT and EMDR. If you are offered alternative treatments, these should be recommended by a healthcare professional with expertise in the treatment of PTSD. Or they should be recommended as part of a formal clinical trial.
Unfortunately, it can take some time to access talking therapies through the NHS. This will depend on where you live and what is available in your area.
In the meantime, you might find it helpful to use self-help materials. Ask your GP if they have any materials they can recommend. Or you can look at NHS Scotland’s PTSD and complex PTSD self-help guide.
Medication
Antidepressants
Your doctor might suggest that you start taking antidepressants. These can be helpful if:
- you are waiting for psychological therapy
- you have tried psychological therapy to treat your PTSD and this hasn’t worked
- you do not want to do psychological therapy.
Selective serotonin reuptake inhibitors (SSRIs) are a type of antidepressant that can help to reduce PTSD symptoms. If you are also experiencing depression, antidepressants can help with this.
Other medications
If SSRIs do not work for you, you may be offered a different medication, such as other antidepressants or an antipsychotic.
Antipsychotic medications are used to treat several different mental health conditions. Antipsychotics are also known as major tranquilisers. Like SSRI antidepressants, antipsychotics can help to reduce your PTSD symptoms. It is important to know that if you have PTSD and are offered an antipsychotic this does not mean that you have psychosis or another serious (non-PTSD) mental health condition.
Other medications will usually need to be prescribed by a psychiatrist to start with. They should discuss the pros and cons of each type of medication with you.
Medication is not a first-line treatment for PTSD. However, appropriate medication can make it easier for you to engage with other treatment and support, like psychological therapies.
What treatment works best?
There is evidence that TF-CBT and EMDR are the best first-line therapies for PTSD. Medication can be helpful for those who do not want talking therapies or who cannot access them easily.
Which treatment should I receive first?
Trauma-focused psychological therapies (TF-CBT or EMDR) should be offered before medication, wherever possible. This is according to guidelines produced by the National Institute for Health and Care Excellence (NICE). These therapies also help as part of the treatment of complex PTSD, which we talk about later in this resource.
There are several things that you can do to support your recovery if you have PTSD. If you have a therapist, they should support you with these techniques and help you to approach them at a pace that feels manageable for you:
Keeping to your routine
If possible, try to get back to or stay in your usual routine. Keeping your life as unchanged as possible can give you a sense of structure and grounding.
Talk to someone you trust
You shouldn’t feel like you have to talk about what happened with just anyone. However, talking to someone you trust can help you to process your feelings in a safe space. If other people were involved in the traumatic event you experienced, it might also help to speak to one of them. Only do this if it is not too distressing for you.
Seek out peer support
To do this, you could find a charity that works with people who have experienced the kinds of things that you have. Ask if they have any ‘peer support’ opportunities or support groups. We have suggested some charities at the end of this resource that you might find helpful.
Try relaxation exercises
Try self-led meditation and mindfulness exercises to relax. Whilst finding ways to relax when you have PTSD can be challenging, it can help you to gain some control over your symptoms. However, relaxation techniques are not a cure and should be part of a wider range of support methods and skills you use to recover. It’s best to speak to your therapist about exercises or activities that might work for you.
Consider returning to work or school
If you feel able, it can help to return to work, school or university. While taking time off can be very valuable after the event, being off for a long time can negatively affect your mental health and self-esteem. Working or attending school or university can give you a sense of routine and purpose. This can help with your recovery.
Try to avoid being in situations where you might be exposed to further trauma or intense stress. If possible, working in a supportive, lower-stress environment is best while you are recovering. Speak with your manager about any reasonable adjustments that could be made to help you through this difficult time.
Eat and exercise regularly
Try to eat when you usually would, even if you don’t feel hungry or motivated to prepare meals or feed yourself. If you feel able, try to exercise regularly. This can also help you to feel more tired when it’s time for you to sleep. You can find out more about sleep in our sleeping well resource.
Spend time with others
Taking time to be with the people you care about can give you a sense of support. It is worth being around other people even if you don’t want to talk about what has happened. Even a phone call or text message can help you to feel connected.
Expect to get better
Try to hold onto the belief that recovery is possible. Having hope can support your healing, but try not to put pressure on yourself to get better quickly. Try to be kind to yourself during this time.
Go back to where the traumatic event happened
You might find it helpful to go back to, or at least near to, where the traumatic event happened. You should only do this when you feel ready. It can be helpful to talk to your therapist or doctor if you are planning to do this, so they can support you with this step. It is important that returning to where a traumatic event happened is planned carefully. You might find it helpful to go with someone that you trust.
Things to avoid
There are some things you might want to avoid, or be conscious of, while you are recovering. Doing the ‘right thing’ can be really challenging and you shouldn’t feel guilty if you find yourself doing any of these things. Try your best to avoid:
- Self-criticism – PTSD symptoms are not a sign of weakness. They are a normal reaction to terrifying experiences. There are plenty of strong, resilient people who have developed PTSD, such as emergency responders and war journalists.
- Keeping your feelings to yourself – If you have PTSD, don’t feel guilty about sharing your thoughts and feelings with others. Talking about how you are feeling can support your recovery, and people who care for you will want to help if they can.
- Expecting things to go back to normal straight away – Treatment for PTSD can take time, and you might have ups and downs. Try not to expect too much of yourself too quickly, but don’t lose hope. With treatment and support, things will improve.
- Staying away from other people – Spending lots of time on your own can increase feelings of isolation and make you feel worse. Try to spend time with other people if you can, and remember that you don’t have to talk about what happened.
- Alcohol and smoking – While alcohol can help you relax in the moment, over time it can make you feel much worse. Coffee and nicotine can act as stimulants which might make you feel worse if you are experiencing symptoms associated with PTSD.
- Getting overtired – PTSD can make sleeping difficult. Try as much as possible to stick to your usual sleeping routine and avoid staying up late, as this can make you feel worse. You can find out more in our resource on sleeping well.
Finally, you might also want to be careful when driving and if you feel unsafe to drive you should let the DVLA know. People can be more prone to accidents after something traumatic has happened.
Some people develop a condition called complex post-traumatic stress disorder (complex PTSD). This is often a result of experiencing a sustained event, or series of events, that are extremely threatening or horrifying. These events can happen during childhood or as an adult. These events will often have been difficult or impossible to easily escape from or avoid.
Examples of events that can lead to complex PTSD include:
- prolonged domestic violence
- repeated childhood sexual or physical abuse
- torture
- living in a war zone
- genocide campaigns
- slavery.
As well as the symptoms of PTSD, if you have complex PTSD you will also:
- have extremely negative beliefs about yourself as 'diminished', 'defeated' or 'worthless'
- find it extremely difficult to regulate your emotions and emotional responses
- find it extremely difficult to sustain relationships and feel close to other people.
Lack of trust in other people and the world in general is common in people with complex PTSD. Treatment for complex PTSD often takes longer to allow people to develop a secure relationship with a therapist. The work someone with complex PTSD does with a therapist will often happen in three stages. However, you might not need to do all of these stages or do them in order, and you might repeat stages.
Stage 1: Stabilisation
Stabilisation is designed to help you to regain control over your anxiety and your re-experiencing symptoms. For example, intrusive thoughts or flashbacks.
In the stabilisation stage you will:
- learn to trust your therapist
- learn to understand and manage your feelings of distress and detachment
- learn ‘grounding’ techniques. These can help you to concentrate on ordinary physical feelings. This can help to remind you that you are living in the present and not the past.
Stabilisation can help you to 'disconnect' your feelings of fear and anxiety from the memories and emotions that trigger them. This can help to make these memories less frightening and intense.
Sometimes stabilisation might be the only help that is needed.
Stage 2: Trauma-focused therapies
Once you feel able to trust your therapist, and have better control over some of your symptoms, treatment will focus on dealing with the trauma. This usually includes TF-CBT or EMDR, which will help you to process your traumatic experiences.
Other psychotherapies may be helpful alongside TF-CBT or EMDR if some of your symptoms are difficult to deal with.
Your therapist will be careful not to push you too fast during this phase of treatment to prevent making the situation worse for you.
Stage 3: Reintegration or reconnection
As your trauma symptoms improve, your therapist will support you to gradually return to a more routine way of life. This stage usually focuses on helping you to adjust to the real world now that you are no longer in the dangerous situation you were in before. This can feel both scary and hopeful, especially at first.
During this process, you should begin to reclaim your sense of self. You will learn to see yourself as a person with rights and the freedom to make choices.
Reintegration will help you to:
- Relate compassionately to yourself and others.
- Re-establish trust in yourself and others.
- Empower you to reengage in friendships, intimate relationships and activities that promote your health and wellbeing. This might include work, if you are not already working.
Unfortunately, as with PTSD, it can take some time to access talking therapies for complex-PTSD. This will depend on where you live and what is available in your area.
Medication
As with PTSD, antidepressants or other medication can be used to treat complex PTSD. Antidepressants can be used:
- alongside psychological therapy
- instead of psychological therapy
- if you are waiting for psychological therapy, or it is not available
- if psychological therapy is not working for you.
It may help to have a psychiatrist review your medication as well.
Self-help
The section earlier in this resource called ‘How can I support myself?’ covers things you can do to help yourself if you have complex PTSD.
If you know someone who has just experienced a traumatic event, there are some things you might want to look out for. These things could be signs that they are struggling to cope:
- Changes in their behaviour – Unusual poor performance at work, lateness, taking sick leave or minor accidents.
- Changes in their emotions – Unusual anger, irritability, depression, lack of interest or a lack of concentration.
- Changes in their thoughts – Dwelling on threats, fears or negative views of the future.
- Unexpected physical symptoms – Such as breathlessness, agitation, jumpiness or stomach aches.
If you think someone might be showing signs of PTSD, you could encourage them to speak to their GP, or another healthcare professional they trust. If you do not feel close enough to them to do this, you might want to speak to someone they are close to, who could do this instead.
It may also help for them to look at information about PTSD, such as this resource. This might help them identify the difficulties they are having and what to do about them.
Things you can do
The following things can help to support someone who has been through a traumatic experience:
Be there
Offer to spend time with them. If they don’t want to see you, it can help to let them know that you will still be there if they change their mind. While you should avoid pressuring them, you may need to ask them more than once before they accept your support.
Listen
Try not to pressure them into sharing what happened to them if they do not feel able to share. If they do want to talk, try to listen and don’t interrupt or share your own experiences. While sharing your own experiences can be done with good intentions, it can sometimes feel invalidating.
Ask general questions
If you do ask questions, try to make them general and non-judgmental. For example, you might want to ask, ‘Have you spoken to anyone else about this?’ or ‘Can I help you to find some extra support?’
Offer practical help
They may find it more of a struggle to look after themselves and keep to a daily routine. You could offer to help with practical things, such as cleaning or preparing a meal.
Look after yourself
If you’re supporting someone, make sure you are looking after yourself too. Supporting someone who has experienced a traumatic event can be emotionally challenging.
Things to avoid
Telling them you know how they feel
Even if you have experienced something similar, people experience situations very differently. It can be unhelpful to make comparisons. Remember, even if you know a lot about what someone has experienced, they might not have told you everything. Because of this, the comparisons you are making might not be accurate.
Telling them they are lucky to be alive or uninjured
People who have experienced traumatic events often won’t feel lucky. People can sometimes feel guilty for:
- being alive if others have died
- not being injured
- not being injured as badly as others were.
Telling them they have been lucky can encourage them to make comparisons between themselves and others. Or it can cause them to feel ashamed by the response they have had.
Minimising their experience
Avoid suggesting it could have been worse, even if you are trying to make them feel better. This can make people feel as though their feelings aren’t justified.
Making suggestions
Avoid making suggestions, even if you have found that these have worked for you in the past. All people are different and the person you know may have already tried what you are suggesting. If you are unsure if the person you are speaking to is looking for suggestions, ask them.
- Overview of PTSD, NHS – Information from the NHS on PTSD.
- Overview of complex PTSD, NHS – Information from the NHS on complex PTSD.
- PTSD, Mind – Information from the charity Mind on PTSD and complex PTSD.
- How can friends and family help? Mind – Information from the charity Mind on how you can help someone you know who has PTSD.
- Useful contacts, Mind – Links to other charities and organisations that offer support to people with PTSD.
Helplines
- Samaritans – Samaritans is a charity that offers listening and support services to anyone who needs them.
- Shout – Shout is a free, confidential and 24/7 text messaging service for anyone in the UK who needs support.
Charities
Here are some charities that offer support to people who experience PTSD or traumatic events:
- PTSD UK – A UK charity dedicated to raising awareness of PTSD.
- Combat Stress – A UK charity for veterans’ mental health.
- Cruse Bereavement Care – A charity offering support for bereaved people in England, Wales and Northern Ireland.
- Cruse Bereavement Care Scotland – A charity promoting the well-being of bereaved people in Scotland.
Rape Crisis – There are three Rape Crisis charities that support people across the UK who have been affected by sexual violence and abuse:
Victim Support – There are three Victim Support charities that support people across the UK who have been victims of crime and traumatic incidents:
There are many organisations that support people who have gone through different experiences, and we have not included all of them here.
This information was produced by the Royal College of Psychiatrists’ Public Engagement Editorial Board (PEEB). It reflects the best available evidence at the time of writing.
Special thanks to PTSD UK, who kindly offered their feedback on this resource.
Expert editor: Professor Neil Greenberg
Experts by experience: Autumn Foord, Brian Hayden and Ellie Wildbore
Full references for this resource are available on request.
Published: March 2026
Review due: March 2029
© Royal College of Psychiatrists










